"A healthcare facility without WASH is not a healthcare facility."
- Dr. Maria Neira, director of Public Health and Environment, World Health Organization
"If you can't do the basics forget the rest. Prevention, prevention, prevention."
- Dr. Tedros Adhanom Ghebreyesus, Director-General, World Health Organization
"Today, I am using the launch of the Water Action Decade to make a global call to action for water, sanitation and hygiene – or WASH -- in all health care facilities… We must work to prevent the spread of disease. Improved water, sanitation and hygiene in health facilities is critical to this effort.”
- UN Secretary-General António Guterres on World Water Day 2018
MORE NEWS:
- Dr. Maria Neira, director of Public Health and Environment, World Health Organization
"If you can't do the basics forget the rest. Prevention, prevention, prevention."
- Dr. Tedros Adhanom Ghebreyesus, Director-General, World Health Organization
"Today, I am using the launch of the Water Action Decade to make a global call to action for water, sanitation and hygiene – or WASH -- in all health care facilities… We must work to prevent the spread of disease. Improved water, sanitation and hygiene in health facilities is critical to this effort.”
- UN Secretary-General António Guterres on World Water Day 2018
MORE NEWS:
- Global leaders speak out for WASH in healthcare, in this must see video compilation
- WHO passes a landmark Resolution to improve WASH in healthcare facilities around the world: click here for more
- 100 organizations make wide-ranging commitments to WASH in Healthcare Facilities: click here to learn more
- Faiths gather for historic meeting on WASH in Healthcare: click here for more
|
Upwards of 50% of healthcare facilities are operated by faith-based organizations in some countries. No where could we have a greater impact on human health and suffering than here.
During the Middle Ages, life-expectancy was measured in the teens, not decades, because much of the world lived in filth: poor hygiene, practically no sanitation and unsafe water. Epidemics and diseases like bubonic plague, typhus, smallpox and tuberculosis (“consumption”) took a massive toll on humanity. Little improvement was made until the 19th Century when the Industrial Revolution, germ theory of disease, and a nurse named Florence Nightingale became the driving force for hospital reform. She convinced the world that improving hygiene and sanitation, as well as having trained professional nurses tend to the sick, were necessities. Ebola and COVID-19 have re-enforced this lesson still not learned, when all around the world healthcare staff and patients cannot wash their hands. WASH is Water, Sanitation & Hygiene Assuring access to sustainable clean water, toilets, soap, basic sanitation and hygiene practices inside hospitals and health clinics is the foundation for safe and dignified healthcare everywhere. Maternal, newborn and child health, pandemic prevention, antibiotic resistance, Infection Prevention and Control (IPC), and the call for Universal Health Coverage (UHC) all require WASH in healthcare. Multiple Sustainable Development Goals (SDGs) cannot be achieved without it. |
 This ward is not from the 1800s. Photo: Oxfam International This ward is not from the 1800s. Photo: Oxfam International
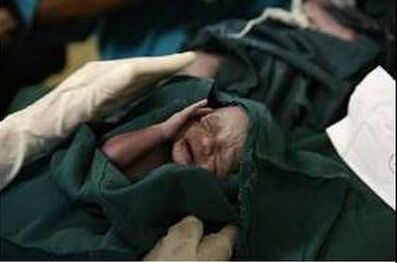
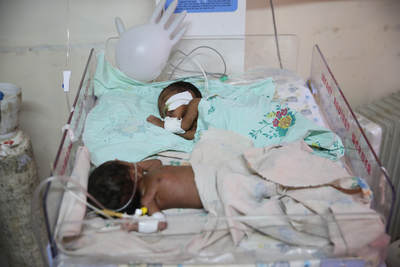
Well into the 21st century, hospitals and healthcare facilities look like something from the 1800s. As medicine travels across bionics and gene therapy into string theory and nanotechnology, the most important discovery that can save millions of lives is left behind. Here's the data you need to know: Every year, 17 million women in developing countries give birth in healthcare facilities without adequate water, sanitation and hygiene. One million newborn deaths annually are associated with unclean births, with infections accounting for 26% of neonatal deaths, and 11% of maternal deaths. In 2019, WHO/UNICEF issued the first baseline global assessment of Water, Sanitation, Hygiene (WASH) in healthcare facilities (HCFs). (JMP, 2019). Data from 560,000 HCFs revealed devastating conditions:
|
NEWBORNS AND NEW MOTHERS
ARE MOST VULNERABLE
WASH and safe births:
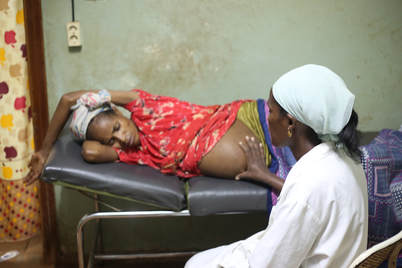
“Encouraging women to give birth in healthcare facilities is one of the key strategies for reducing maternal mortality. Yet even in the very facilities that are set up to serve their communities with healthcare and welcome new life into the world, there is often no constant clean water supply, functioning toilets or handwashing facilities.” click here to read more...
“Bring your own” birthing kit:
“In some cases, women giving birth must buy their own ‘clean birth kit’, which includes a plastic sheet and gloves to compensate for the lack of adequate hygiene provision in maternity units.” click here to read more...
Newborns and sepsis:
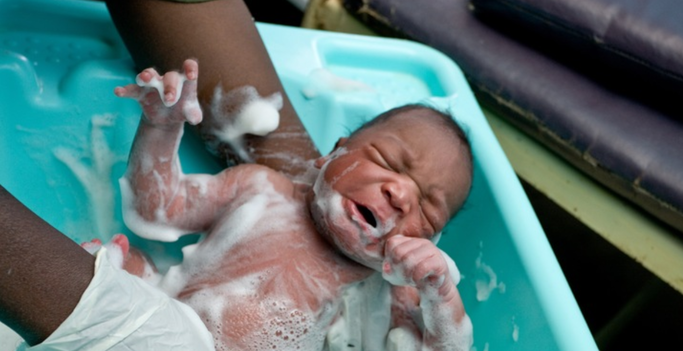
“8% of maternal mortality is caused by sepsis. A failure to make sure that a woman has a clean place to give birth, that a midwife, birth attendant or doctor has clean hands when helping her deliver, and that the blade which separates the child from his mother by cutting the umbilical cord is clean puts a baby at risk. The absence of sufficient infection prevention and control measures in healthcare facilities should be of particular concern to those attempting to redress the slow progress to reduce maternal mortality globally.” click here to read more...
50 % of the health burden of malnutrition is attributable to WASH:
“Diarrhea is deadly. 1.5 million people die every year from diarrheal diseases (including cholera); 90% are children under 14, mostly in developing countries. 88% of diarrhea is attributed to unsafe water supply, inadequate sanitation and hygiene. As diarrhea causes undernutrition, it creates a vicious cycle by also reducing a child’s resistance to subsequent infections; repeated bouts of diarrhea can negatively impact children’s physical and cognitive development.” click here to read more...
Up to 1:2 surgical patients can leave a hospital with an infection they did not have upon arrival:
“In some developing countries up to one in every two patients (45.6%) left hospital with an infection they had not had on arrival.”
click here to read more...
For more information:
WATER WORKS:
- Improved water supply reduces diarrhea morbidity by 21%.
- Improved sanitation reduces diarrhea morbidity by 37.5%.
- Simply handwashing with soap can reduce diarrheal episodes by about 45%.
- When children wash their hands, healthy global development indicators like height, weight, and social skills increase as do child well‐being and social productivity.
CASE STUDY:
VILLAGE HEALTH PARTNERSHIP
"I recently found myself in a packed labor and delivery ward. When an unexpected twin was born not breathing, we had no choice. With almost no protective gear, two nurses I’d brought with me jumped in and saved the baby. Covered with blood, we just had to hope no mother or child we came in contact with that day was infected with HIV, hepatitis... We had no way to clean up because this massive, overcrowded hospital that serves 2.5 million people, had had no water in six weeks.”
- Margaret “Migs” Muldrow, MD Internal Medicine and Dermatology, Founder, Village Health Partnership
VILLAGE HEALTH PARTNERSHIP
"I recently found myself in a packed labor and delivery ward. When an unexpected twin was born not breathing, we had no choice. With almost no protective gear, two nurses I’d brought with me jumped in and saved the baby. Covered with blood, we just had to hope no mother or child we came in contact with that day was infected with HIV, hepatitis... We had no way to clean up because this massive, overcrowded hospital that serves 2.5 million people, had had no water in six weeks.”
- Margaret “Migs” Muldrow, MD Internal Medicine and Dermatology, Founder, Village Health Partnership
Village Health Partnership seeks to improve health systems in rural Ethiopia. A visit to 16 rural healthcare facilities found, without exception, every hospital and clinic with periods of limited or no water and not one had the basic combination of clean water, access to hand-washing facilities with soap in exam rooms (including labor and delivery), and sanitation. Ethiopia is in no way alone. It's a problem common throughout low- and middle- income countries.
Photos by Haik Kocharian for Village Health Partnership (VHP)
Photos by Haik Kocharian for Village Health Partnership (VHP)
|
“Ethiopians work very hard to solve their issues. They are also deeply ashamed of the level of poverty and won’t talk about sanitation for fear outsiders will react with judgment. I have anything but judgment. I have hope. Though one of the most desperate places in terms of maternal and child health, mortality rates are dropping in areas where international assistance and the Ethiopian government have reach. And we’re learning that local commitment is vital to creating sustainable health systems. But it seems to me that we shouldn’t have to learn that water is, too.” - Dr. Margaret “Migs” Muldrow |
|
|
"A darling, petite young woman with a beautiful smile on the outside, Mecca’s reality is a daily onslaught of pain and shame due to a completely preventable injury of pregnancy, afflicting a million women and resulting in untold stillbirths. I was in Ethiopia with a project focused on the appalling absence of Water/Sanitation/Hygiene (WASH) in health-care facilities. It’s a global health scandal impacting hundreds of thousands of clinics and hospitals around the world. But I hadn’t anticipated Meeting Mecca..." |
VHP founder, Dr. Migs Muldrow (far left) and Susan Barnett (far right), founder, Faiths for Safe Water, interview Mecca outside her home. Read her story.
AMR IS SCARY. REALLY SCARY.
If we don’t take global action to prevent infections, and keep relying on antibiotics to cure infections, we will return to the days before we had any antibiotics.
"Our modern medical system is built on effective antibiotics. If our antibiotics stop working, if bacteria become resistant to most of them, medicine will be in trouble.”
- Eili Klein, Center for Disease Dynamics, Economics and Policy
Anti-microbial resistance, AMR, means many of the common antibiotics we’ve all come to rely on are no longer effective. Drug resistance is a rapidly growing global threat. Drug-resistant diseases can cause longer and more complicated illnesses, more doctor visits, the need for stronger and more expensive drugs, and more deaths. The CDC uncovered new "nightmare bacteria" — resistant to almost every drug, and particularly deadly to the elderly and people with chronic illnesses. Up to half of these infections are fatal.
Yet, 2000 to 2015 saw a 65% rise in worldwide consumption of the drugs; on average, especially among wealthier nations. "Unrestrained antibiotics use is the key reason drug-resistant infections now kill more than half a million people a year worldwide," according to a recent study co-authored by Eli Klein of the Center for Disease Dynamics, Economics and Policy in Washington. About 2 million Americans are sickened by antibiotic-resistant bacteria each year and 23,000 die, according to the CDC.
|
But what about the antibiotics of tomorrow? Pharmaceutical companies have continually withdrawn from developing new antibiotics. In 1990, there were at least 18 large pharmaceutical companies actively developing antibiotics. Today, there are four. Concern has led England’s chief medical officer to recently add antimicrobial resistance to the UK’s national risk register of civil emergencies. Five years ago, Dame Sally Davies warned of an “apocalyptic scenario” where people die of common infections and simple operations because antibiotics no longer work. Davies recently told The Guardian, “The importance of clean water, sanitation and vaccination must not be forgotten to avoid infections occurring in the first place.” More in The Guardian. Resistance can also spread between microorganisms. Using antimicrobials in any one sector (human health, aquaculture, agriculture or on crops) can result in unintended exposure in other sectors. AMR can undermine not only human health, but also animal health, crop health and ecosystem health. |
Every infection prevented is one that needs no treatment. We must prevent infections and better manage antibiotics: |
PREVENTING PANDEMICS
THE 2014 EBOLA OUTBREAK
The lack of access to water, soap and basic sanitation was a key reason why Ebola not only killed some 11,00 people, it was 103-fold higher in healthcare workers in Sierra Leone than in the general population, 42-fold higher in Guinea health workers, and the reason why Liberia lost eight percent of its health workforce.
These professionals are also our frontline defense against pandemics.
When the WHO published its top 10 threats to global health in 2019, 4 of the 10 had one thing in common — they directly relate to the absence of WASH in hospitals and healthcare facilities: Pandemic influenza, AMR, Ebola and other high-threat pathogens and haemorrhagic fevers, Zika, Nipah, Middle East respiratory syndrome coronavirus (MERS-CoV), Severe Acute Respiratory Syndrome (SARS) and disease X, which represents the need to prepare for an unknown pathogen that could cause a serious epidemic.
THEN CAME COVID-19 AND HEALTHCARE WORKERS STILL CANNOT WASH THEIR HANDS.
These professionals are also our frontline defense against pandemics.
When the WHO published its top 10 threats to global health in 2019, 4 of the 10 had one thing in common — they directly relate to the absence of WASH in hospitals and healthcare facilities: Pandemic influenza, AMR, Ebola and other high-threat pathogens and haemorrhagic fevers, Zika, Nipah, Middle East respiratory syndrome coronavirus (MERS-CoV), Severe Acute Respiratory Syndrome (SARS) and disease X, which represents the need to prepare for an unknown pathogen that could cause a serious epidemic.
THEN CAME COVID-19 AND HEALTHCARE WORKERS STILL CANNOT WASH THEIR HANDS.
FAITH COMMUNITY CALL-TO-ACTION:
No community is better positioned to lead because faith-based communities run up to 50% of healthcare facilities in some countries. If we are truly committed to preventing suffering, illness and disease, and improving health outcomes, then we must direct greater focus to sustainable WASH in healthcare facilities.
Sustainable WASH in healthcare facilities will require systemic change, and integrating WASH into existing health initiatives like infection prevention and control (IPC) and antimicrobial resistance (AMR), maternal and child health (MCH), quality of care, and universal health coverage (UHC). It will require expertise and support from clinicians, public health professionals, engineers, plumbers, government officials, researchers, donors and more to achieve the goal of universal coverage.
Key stakeholders are working with the senior leadership of the UN, especially WHO and UNICEF, to respond by developing action plans and furthering the global campaign to address this urgent issue. Our faith-based organizations are key stakeholders and our leadership can help prioritize and coordinate vital multi-sector cooperation.
Know an organization that could benefit from more field and technical information about WASH in Healthcare Facilities?
Visit the NEW WASHinHCF.org for a growing list of shared resources.
No community is better positioned to lead because faith-based communities run up to 50% of healthcare facilities in some countries. If we are truly committed to preventing suffering, illness and disease, and improving health outcomes, then we must direct greater focus to sustainable WASH in healthcare facilities.
Sustainable WASH in healthcare facilities will require systemic change, and integrating WASH into existing health initiatives like infection prevention and control (IPC) and antimicrobial resistance (AMR), maternal and child health (MCH), quality of care, and universal health coverage (UHC). It will require expertise and support from clinicians, public health professionals, engineers, plumbers, government officials, researchers, donors and more to achieve the goal of universal coverage.
Key stakeholders are working with the senior leadership of the UN, especially WHO and UNICEF, to respond by developing action plans and furthering the global campaign to address this urgent issue. Our faith-based organizations are key stakeholders and our leadership can help prioritize and coordinate vital multi-sector cooperation.
Know an organization that could benefit from more field and technical information about WASH in Healthcare Facilities?
Visit the NEW WASHinHCF.org for a growing list of shared resources.
WATER IS LIFE:
BUT TOO OFTEN IT IS NOT:
PREVENTION IS
AS CLEAR AS CLEAN WATER.
Faiths for Safe Water's Faith-based Resources offer lots of ways for families, students and congregations to make our shared religious symbol a source of health and life for all.
LET'S MAKE EVERY DAY
WORLD WATER DAY
Contact:
|